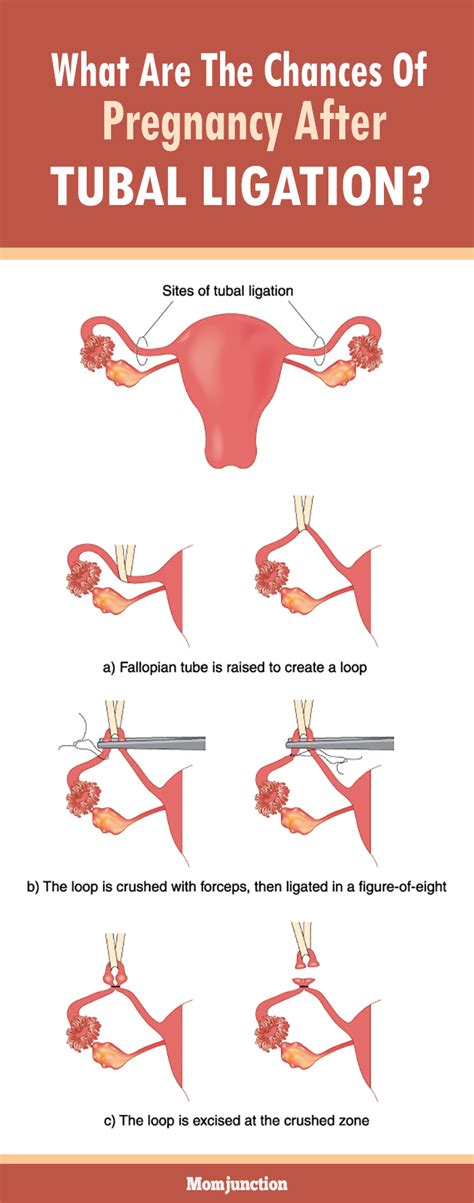
Tubal ligation is a surgical procedure that blocks the fallopian tubes, preventing pregnancy. It is one of the most effective methods of contraception, but no method is 100% effective. The question of “how common is it to get pregnant after tubal ligation” is a valid concern for women considering this procedure.
The risk of pregnancy after tubal ligation is low, but it is not zero. Studies have shown that the failure rate of tubal ligation is between 0.5% and 1.5%. This means that for every 100 women who have a tubal ligation, 0.5 to 1.5 will become pregnant.
The risk of pregnancy after tubal ligation is highest in the first year after the procedure. This is because the fallopian tubes may still be healing and may not be completely blocked. The risk of pregnancy decreases over time, but it is never completely eliminated.
How Common Is It to Get Pregnant After Tubal Ligation
Pregnancy after tubal ligation, while uncommon, highlights crucial aspects that influence its likelihood. These aspects encompass factors related to the procedure, the individual’s health, and other relevant considerations.
- Tubal ligation technique
- Surgeon’s experience
- Patient’s age
- Smoking
- Underlying medical conditions
- Time since procedure
- Ectopic pregnancy risk
- Ovarian function
- Emotional impact
Understanding these aspects is vital in assessing the likelihood of pregnancy after tubal ligation. For instance, the surgeon’s experience and the technique used can impact the success rate of the procedure. Additionally, factors like age, smoking, and medical conditions can influence the chances of pregnancy. It’s crucial to discuss these aspects with a healthcare professional to make an informed decision about tubal ligation and its potential outcomes.
Tubal ligation technique
The technique used for tubal ligation can influence the likelihood of pregnancy after the procedure. Different techniques vary in their effectiveness and potential complications.
- Type of surgery
Laparoscopic surgery, which involves making small incisions in the abdomen, is generally considered to be more effective than minilaparotomy, which involves making a larger incision. - Method of tubal occlusion
There are several methods of tubal occlusion, including cutting, burning, or clipping the fallopian tubes. The choice of method may depend on the surgeon’s preference and the patient’s anatomy. - Bilateral vs. unilateral ligation
Bilateral tubal ligation involves occluding both fallopian tubes, while unilateral ligation involves occluding only one tube. Bilateral ligation is more effective in preventing pregnancy, but it is also a more invasive procedure. - Post-operative care
Proper post-operative care can help to reduce the risk of complications, such as infection and bleeding, which can affect the success of the tubal ligation.
The choice of tubal ligation technique should be made in consultation with a healthcare professional, who can discuss the risks and benefits of each technique and help the patient make an informed decision.
Surgeon’s experience
The experience of the surgeon performing a tubal ligation can influence the likelihood of pregnancy after the procedure. Surgeons who have performed a high volume of tubal ligations are generally more skilled and have a lower complication rate.
- Training and certification
Surgeons who have specialized training and certification in laparoscopic surgery are generally more proficient in performing tubal ligations.
- Number of procedures performed
Surgeons who have performed a high number of tubal ligations are more likely to be proficient in the procedure and have a lower complication rate.
- Patient outcomes
Surgeons who have a history of good patient outcomes are more likely to be skilled in performing tubal ligations.
- Experience with different techniques
Surgeons who are experienced with different techniques of tubal ligation are more likely to be able to choose the best technique for each patient.
Choosing a surgeon who is experienced in performing tubal ligations can help to reduce the risk of pregnancy after the procedure.
Patient’s age
A woman’s age is a critical factor in determining the likelihood of pregnancy after tubal ligation. The risk of pregnancy increases with age, as the fallopian tubes become less elastic and more likely to recanalize, or reopen.
For women under the age of 35, the risk of pregnancy after tubal ligation is about 0.5%. This risk increases to about 1% for women between the ages of 35 and 40, and to about 2% for women over the age of 40.
There are several reasons why age increases the risk of pregnancy after tubal ligation. First, as women age, their fallopian tubes become less elastic. This makes it more difficult for the tubal ligation to completely block the tubes, and it increases the risk of recanalization.
Second, as women age, they are more likely to have other medical conditions, such as obesity and diabetes, which can increase the risk of pregnancy after tubal ligation.
Finally, as women age, they are more likely to have had multiple pregnancies, which can also increase the risk of pregnancy after tubal ligation.
Smoking
Smoking is a significant risk factor that increases the likelihood of pregnancy after tubal ligation. Women who smoke are more likely to have their fallopian tubes recanalize, or reopen, after tubal ligation, which can lead to pregnancy.
There are several reasons why smoking increases the risk of pregnancy after tubal ligation. First, smoking damages the fallopian tubes, making them more likely to recanalize. Second, smoking increases inflammation in the body, which can also contribute to tubal recanalization.
There is a clear dose-dependent relationship between smoking and the risk of pregnancy after tubal ligation. The more a woman smokes, the greater her risk of pregnancy. For example, women who smoke one pack of cigarettes per day have a 2% risk of pregnancy after tubal ligation, compared to a 0.5% risk for women who do not smoke.
Smoking cessation is the most effective way to reduce the risk of pregnancy after tubal ligation. Women who quit smoking before having a tubal ligation have a lower risk of pregnancy than women who continue to smoke.
Underlying medical conditions
Underlying medical conditions can increase the risk of pregnancy after tubal ligation. These conditions can affect the fallopian tubes, making them more likely to recanalize, or reopen, after tubal ligation.
- Pelvic inflammatory disease (PID)
PID is an infection of the female reproductive organs. It can damage the fallopian tubes, making them more likely to recanalize after tubal ligation.
- Endometriosis
Endometriosis is a condition in which tissue similar to the lining of the uterus grows outside the uterus. This tissue can block the fallopian tubes, making them more likely to recanalize after tubal ligation.
- Uterine fibroids
Uterine fibroids are noncancerous growths in the uterus. They can distort the uterus and fallopian tubes, making it more difficult for tubal ligation to be successful.
- Adenomyosis
Adenomyosis is a condition in which the tissue that lines the uterus grows into the muscular wall of the uterus. This can weaken the uterus and make it more likely for the fallopian tubes to recanalize after tubal ligation.
Women with any of these underlying medical conditions should discuss the risks and benefits of tubal ligation with their doctor before making a decision about the procedure.
Time since procedure
The time interval elapsed since a tubal ligation procedure significantly influences the likelihood of subsequent pregnancy. Understanding the impact of time on the procedure’s efficacy is integral when assessing the overall risk of pregnancy.
- Early Post-Operative Period
Immediately following the procedure, the risk of pregnancy is at its lowest, as the fallopian tubes are freshly ligated or blocked. However, within the first few months, the risk may gradually increase due to potential tissue healing and tubal recanalization.
- One to Five Years Post-Procedure
During this period, the risk of pregnancy remains relatively low, typically within the range of 0.5% to 1%. However, certain factors, such as smoking or underlying medical conditions, may elevate the risk.
- Five to Ten Years Post-Procedure
As more time passes, the risk of pregnancy gradually increases. This is primarily attributed to the potential for spontaneous tubal recanalization, where the blocked fallopian tubes naturally reopen over time.
- Long-Term (>Ten Years Post-Procedure)
In the long term, the risk of pregnancy after tubal ligation continues to rise, albeit remaining below the pre-procedure risk. Regular monitoring and follow-up with a healthcare provider are crucial to assess any changes or potential complications.
Overall, the time elapsed since a tubal ligation procedure plays a critical role in determining the likelihood of pregnancy. While the risk is generally low, it is not entirely eliminated and may vary depending on individual factors and the specific time frame considered.
Ectopic pregnancy risk
Understanding the risk of ectopic pregnancy is crucial when discussing “how common is it to get pregnant after tubal ligation.” An ectopic pregnancy occurs when a fertilized egg implants outside the uterus, most commonly in the fallopian tube. This condition can be life-threatening and requires prompt medical attention.
- Location
The fallopian tubes are the most common site for ectopic pregnancy after tubal ligation, accounting for over 95% of cases. However, it can also occur in other locations, such as the ovary, cervix, or abdomen.
- Risk factors
Women who smoke, have a history of pelvic inflammatory disease (PID), or have used fertility treatments have an increased risk of ectopic pregnancy after tubal ligation.
- Symptoms
Symptoms of an ectopic pregnancy can include abdominal pain, vaginal bleeding, and irregular periods. However, some women may not experience any symptoms until the ectopic pregnancy ruptures.
- Treatment
Treatment for an ectopic pregnancy typically involves medication or surgery to remove the fertilized egg and repair the affected area. Early diagnosis and treatment are crucial to prevent life-threatening complications.
While the risk of ectopic pregnancy after tubal ligation is low, it is important to be aware of the potential risks and symptoms. Women who experience any of the symptoms of an ectopic pregnancy should seek medical attention immediately.
Ovarian function
Ovarian function plays a crucial role in understanding the likelihood of pregnancy after tubal ligation. The ovaries are responsible for producing eggs and hormones, which are essential for fertility. After tubal ligation, ovarian function continues, but its impact on pregnancy is altered.
- Hormonal production
The ovaries continue to produce hormones, including estrogen and progesterone, which regulate the menstrual cycle and prepare the uterus for pregnancy. After tubal ligation, hormone levels may be slightly lower, but they typically remain within the normal range.
- Egg production
The ovaries continue to produce eggs after tubal ligation. However, since the fallopian tubes are blocked, the eggs cannot reach the uterus for fertilization. This prevents pregnancy from occurring.
- Ovulation
Ovulation is the process by which an egg is released from the ovary. After tubal ligation, ovulation typically continues to occur regularly. However, the eggs are not able to be fertilized and are reabsorbed by the body.
- Age-related changes
As women age, their ovarian function naturally declines. This can lead to a decrease in fertility and an increased risk of pregnancy after tubal ligation. This is because the ovaries produce fewer eggs and the eggs are of lower quality.
Overall, ovarian function continues after tubal ligation, but its impact on pregnancy is significantly reduced. The ovaries continue to produce hormones and eggs, but the eggs cannot reach the uterus for fertilization. As a result, the risk of pregnancy after tubal ligation is very low.
Emotional impact
Tubal ligation is a surgical procedure that blocks the fallopian tubes, preventing pregnancy. It is a highly effective method of contraception, but no method is 100% effective. The emotional impact of an unplanned pregnancy after tubal ligation can be significant.
For many women, an unplanned pregnancy after tubal ligation can be a source of great distress. They may feel overwhelmed, anxious, and uncertain about the future. They may also feel guilty or ashamed, as if they have failed in some way. These emotions can be compounded by the fact that an unplanned pregnancy after tubal ligation is often seen as a medical failure.
The emotional impact of an unplanned pregnancy after tubal ligation can also be felt by the woman’s partner, family, and friends. They may also feel overwhelmed, anxious, and uncertain about the future. They may also feel angry or resentful towards the woman, or towards the medical professionals who performed the tubal ligation.
It is important to remember that an unplanned pregnancy after tubal ligation is not a failure. It is a rare event, but it can happen. If you find yourself in this situation, it is important to seek support from your partner, family, friends, and healthcare providers.
FAQs
This section addresses frequently asked questions regarding the likelihood of pregnancy after tubal ligation, a surgical procedure designed to prevent pregnancy.
Question 1: How common is it to get pregnant after tubal ligation?
The risk of pregnancy after tubal ligation is low, estimated to be between 0.5% and 1.5%. This means that for every 100 women who have a tubal ligation, 0.5 to 1.5 will become pregnant.
Question 2: What factors can increase the risk of pregnancy after tubal ligation?
Factors such as the patient’s age, smoking habits, underlying medical conditions, and the surgical technique used can influence the risk of pregnancy after tubal ligation.
Question 3: What should I do if I become pregnant after tubal ligation?
If you become pregnant after tubal ligation, it is essential to seek prompt medical attention. An unplanned pregnancy after tubal ligation may pose certain risks and require specialized care.
Question 4: What are the treatment options for an ectopic pregnancy after tubal ligation?
An ectopic pregnancy, a pregnancy that occurs outside the uterus, is a potential risk after tubal ligation. Treatment options may include medication or surgery to address the ectopic pregnancy.
Question 5: Can I still get pregnant naturally after tubal ligation has failed?
In some cases, tubal ligation can fail, allowing for a natural pregnancy. However, the likelihood of a successful pregnancy after a failed tubal ligation is generally low.
Question 6: What emotional impact can an unplanned pregnancy after tubal ligation have?
An unplanned pregnancy after tubal ligation can a range of emotions, including distress, anxiety, and uncertainty. It is important to seek support from healthcare providers and loved ones during this time.
Summary:
Understanding the potential risks and emotional impact of pregnancy after tubal ligation is crucial. While the risk is low, factors such as age and lifestyle choices can influence the likelihood of pregnancy. If an unplanned pregnancy occurs, prompt medical attention and emotional support are essential.
Transition to Next Section:
For further insights into the complexities of pregnancy after tubal ligation, we delve into the medical considerations and advancements in surgical techniques.
Tips to Consider Before and After Tubal Ligation
Understanding the likelihood of pregnancy after tubal ligation requires careful consideration. These proactive tips can help you make informed decisions and navigate your reproductive health effectively.
Tip 1: Consult with a qualified healthcare provider: Discuss the procedure, risks, and alternatives thoroughly to ensure it aligns with your reproductive goals.
Tip 2: Choose an experienced surgeon: A skilled surgeon can minimize the risk of complications and improve the success rate of tubal ligation.
Tip 3: Follow post-operative instructions carefully: Adhering to the doctor’s instructions can promote healing and reduce the chances of infection or other complications.
Tip 4: Monitor for symptoms: Pay attention to any unusual symptoms after the procedure, such as pain, bleeding, or discharge, and seek medical attention promptly.
Tip 5: Consider using additional contraception methods: While tubal ligation is highly effective, using additional methods, such as condoms, can further minimize the risk of pregnancy.
Tip 6: Understand the emotional impact: Acknowledge and process the emotional aspects of tubal ligation, including any feelings of loss or uncertainty.
Tip 7: Explore alternative fertility options: If you change your mind about having children in the future, discuss alternative fertility options, such as IVF or adoption, with your healthcare provider.
Tip 8: Maintain regular check-ups: Schedule regular check-ups with your doctor to monitor your overall health and reproductive well-being.
Summary:
These tips empower you to make informed decisions about tubal ligation, minimize risks, and navigate your reproductive health journey confidently.
Transition to the article’s conclusion:
As we conclude our discussion on pregnancy after tubal ligation, it is essential to remember that every woman’s experience is unique. By considering these tips, you can approach this procedure with knowledge and understanding.
Conclusion
Our exploration of “how common is it to get pregnant after tubal ligation” unveils that the risk, while low, is influenced by various factors. Understanding the procedure’s efficacy and potential implications is crucial for informed decision-making.
Key insights include the impact of age, smoking habits, and underlying medical conditions on the likelihood of pregnancy. The choice of surgical technique and the experience of the surgeon also play significant roles. Furthermore, emotional considerations and alternative fertility options should be taken into account.