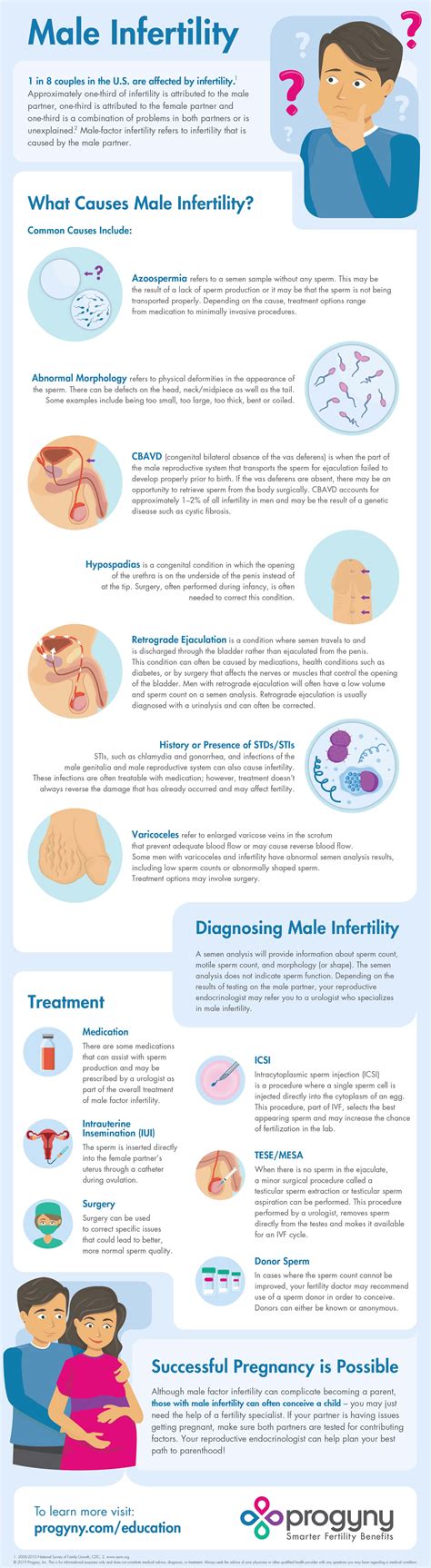
Male Infertility and Pregnancy: A Guide to Causes and Treatment
Male infertility, the inability for a man to conceive a child, affects millions of couples worldwide. Numerous factors can contribute to male infertility, including hormonal imbalances, genetic abnormalities, and lifestyle choices. Understanding the causes and available treatments for male infertility is crucial for couples hoping to start a family.
This article explores the latest advancements in diagnosing and treating male infertility. We’ll cover topics such as:
Identifying the causes of male infertility Various treatment options available The role of assisted reproductive technologies The emotional and psychological impact of infertility Support resources for couples facing infertility. Whether you’re a couple struggling with infertility or a healthcare professional seeking more information, this article provides comprehensive and up-to-date insights into male infertility and its management.
How to Get Pregnant with Male Infertility
Understanding the essential aspects of male infertility is crucial for couples seeking to conceive. These aspects encompass various dimensions, including medical, emotional, and lifestyle factors. Here are 10 key aspects to consider:
- Sperm count
- Sperm motility
- Sperm morphology
- Hormonal imbalances
- Genetic factors
- Lifestyle choices
- Emotional well-being
- Communication
- Support systems
- Treatment options
These aspects are interconnected and can significantly impact a couple’s journey towards parenthood. For instance, low sperm count or poor sperm motility can affect fertilization, while hormonal imbalances may hinder sperm production. Emotional well-being and open communication are equally important, as stress and anxiety can negatively impact fertility. Seeking support from healthcare professionals, family, and support groups can provide invaluable emotional and practical assistance.
Sperm count
Sperm count refers to the number of sperm cells present in a man’s semen. It is a critical factor in male fertility, as a low sperm count can significantly impact a couple’s ability to conceive. The normal sperm count range is between 15 million to 200 million sperm per milliliter of semen. A count below 15 million sperm per milliliter is considered low and can affect fertility.
There are various causes of low sperm count, including hormonal imbalances, genetic factors, lifestyle choices such as smoking and excessive alcohol consumption, and certain medical conditions. Low sperm count can also be a side effect of certain medications or treatments, such as chemotherapy or radiation therapy.
Sperm count is a critical component of male fertility because it directly affects the chances of fertilization. If the sperm count is low, there are fewer sperm available to fertilize the egg. This can make it more difficult for a couple to conceive naturally. In cases of severe oligospermia (very low sperm count), assisted reproductive technologies such as IVF may be necessary to achieve pregnancy.
Sperm motility
Sperm motility is the ability of sperm cells to move and swim. It is a critical component of male fertility, as sperm must be able to navigate through the female reproductive tract to reach and fertilize the egg. Sperm motility is affected by various factors, including the sperm’s shape, size, and energy levels. Poor sperm motility can significantly impact a couple’s ability to conceive.
There are various causes of poor sperm motility, including hormonal imbalances, genetic factors, lifestyle choices, and certain medical conditions. Poor sperm motility can also be a side effect of certain medications or treatments, such as chemotherapy or radiation therapy.
Sperm motility is a critical component of male fertility because it directly affects the chances of fertilization. If the sperm are unable to move or swim properly, they will not be able to reach the egg and fertilize it. This can make it more difficult for a couple to conceive naturally. In cases of severe asthenozoospermia (poor sperm motility), assisted reproductive technologies such as IVF may be necessary to achieve pregnancy.
Understanding the connection between sperm motility and male infertility is crucial for couples seeking to conceive. By addressing factors that may affect sperm motility, such as lifestyle choices or underlying medical conditions, couples can improve their chances of achieving pregnancy.
Sperm morphology
Sperm morphology refers to the size, shape, and structure of sperm cells. It is a critical component of male fertility, as abnormalities in sperm morphology can affect the ability of sperm to fertilize an egg. Normal sperm morphology is characterized by an oval head, a midpiece, and a long, thin tail. Abnormalities in any of these components can impact sperm function and reduce fertility.
There are various causes of abnormal sperm morphology, including genetic factors, hormonal imbalances, lifestyle choices, and certain medical conditions. Abnormal sperm morphology can also be a side effect of certain medications or treatments, such as chemotherapy or radiation therapy.
Sperm morphology is a critical component of male fertility because it directly affects the chances of fertilization. If the sperm are abnormally shaped or structured, they may not be able to swim properly or penetrate the egg’s outer layer. This can make it more difficult for a couple to conceive naturally. In cases of severe teratozoospermia (abnormal sperm morphology), assisted reproductive technologies such as IVF may be necessary to achieve pregnancy.
Hormonal imbalances
Hormonal imbalances are a common cause of male infertility, affecting the production and function of sperm. They can result from various factors, including genetic abnormalities, pituitary gland disorders, and certain medical conditions. Understanding the role of hormones in male fertility is crucial for developing effective treatment plans.
- Testosterone
Testosterone is the primary male sex hormone responsible for sperm production and male reproductive development. Low testosterone levels can lead to decreased sperm count and motility, affecting fertility.
- FSH
Follicle-stimulating hormone (FSH) stimulates the production of sperm in the testes. Abnormal FSH levels can disrupt sperm production and quality.
- LH
Luteinizing hormone (LH) triggers the release of testosterone from the testes. Low LH levels can lead to decreased testosterone production and impaired sperm production.
- Prolactin
Prolactin is a hormone typically associated with breastfeeding in women. However, high prolactin levels in men can suppress testosterone production and affect sperm quality.
Correcting hormonal imbalances is often a key step in treating male infertility. This may involve medication, hormone replacement therapy, or addressing underlying medical conditions that affect hormone production. By restoring hormonal balance, it is possible to improve sperm production and quality, thereby enhancing the chances of successful conception.
Genetic factors
Genetic factors play a significant role in male infertility, affecting the development and function of the reproductive system. These factors can contribute to various aspects of male infertility, including sperm production, quality, and motility.
- Chromosomal abnormalities
Chromosomal abnormalities, such as Klinefelter’s syndrome or Y chromosome microdeletions, can disrupt sperm production and lead to infertility.
- Gene mutations
Mutations in specific genes, such as the CFTR gene associated with cystic fibrosis, can affect the development and function of the male reproductive organs.
- Inherited disorders
Certain inherited disorders, such as Kartagener’s syndrome, can cause structural abnormalities in the reproductive tract or impair sperm motility.
- Genetic predisposition
Some men may have a genetic predisposition to infertility, with a higher likelihood of developing reproductive problems due to inherited genetic traits.
Understanding the genetic factors associated with male infertility is crucial for developing appropriate treatment plans. Genetic counseling and testing can help identify specific genetic abnormalities or predispositions, allowing for targeted interventions and reproductive options. By addressing genetic factors, couples can make informed decisions and explore alternative methods of achieving pregnancy, such as assisted reproductive technologies.
Lifestyle choices
Lifestyle choices significantly impact male fertility and a couple’s ability to conceive. Unhealthy habits, such as smoking, excessive alcohol consumption, drug use, and poor diet, can adversely affect sperm production and quality.
Smoking, for instance, damages sperm DNA and reduces sperm count and motility. Heavy alcohol intake can disrupt hormone production and lead to erectile dysfunction. Illicit drug use, such as marijuana and cocaine, can impair sperm production and function. Additionally, obesity has been linked to decreased testosterone levels and poor sperm quality.
Conversely, adopting a healthy lifestyle can improve male fertility. Maintaining a balanced diet rich in fruits, vegetables, and whole grains provides the body with essential nutrients for sperm production. Regular exercise helps maintain a healthy weight, reduces stress, and improves overall reproductive health. Avoiding excessive alcohol consumption and quitting smoking can significantly enhance sperm quality and increase the chances of conception.
Understanding the connection between lifestyle choices and male infertility empowers couples to make informed decisions and take proactive steps to improve their fertility. By adopting healthier habits, men can optimize their reproductive potential and increase their chances of conceiving a child.
Emotional well-being
Emotional well-being is a critical aspect of male fertility and a couple’s journey toward parenthood. It encompasses a range of psychological and emotional factors that can significantly impact a man’s ability to conceive and the overall success of fertility treatments.
- Stress management
Stress can negatively affect sperm production and quality. Techniques such as exercise, meditation, and therapy can help manage stress levels and improve fertility outcomes.
- Coping with infertility
Infertility can be an emotionally challenging experience. Seeking support from partners, family, friends, or support groups can provide emotional resilience and coping mechanisms.
- Relationship health
A strong and supportive relationship between partners is essential for emotional well-being during infertility. Open communication, empathy, and shared decision-making can strengthen the bond and reduce stress.
- Self-esteem and body image
Infertility can impact a man’s self-esteem and body image. Positive self-talk, focusing on strengths, and seeking professional help if needed can enhance self-worth and improve overall well-being.
Addressing emotional well-being is an integral part of fertility treatment. By understanding and addressing the psychological and emotional challenges associated with male infertility, couples can improve their chances of conceiving and enhance their overall quality of life during this challenging journey.
Communication
Communication is a crucial aspect of navigating the challenges of male infertility and achieving pregnancy. Open and effective communication between partners, healthcare providers, and support networks can significantly impact the journey toward parenthood.
- Partner Communication
Couples need to communicate openly and honestly about their feelings, concerns, and expectations. Sharing the emotional burden and providing support can strengthen their bond and improve coping mechanisms.
- Doctor-Patient Communication
Clear communication with healthcare providers is essential for understanding the diagnosis, treatment options, and potential outcomes. Asking questions, expressing concerns, and actively participating in decision-making can lead to better treatment adherence and outcomes.
- Support Group Communication
Joining support groups or online forums provides a platform for individuals to connect with others going through similar experiences. Sharing knowledge, offering emotional support, and learning from others’ journeys can empower couples and reduce feelings of isolation.
- Self-Communication
Individuals need to engage in self-reflection and communication to understand their own emotions, needs, and limitations. Practicing self-care, seeking professional help when needed, and maintaining a positive mindset can enhance overall well-being and resilience during the infertility journey.
Effective communication fosters understanding, reduces stress, and strengthens the support system for couples facing male infertility. By prioritizing open dialogue, couples can navigate the challenges, make informed decisions, and increase their chances of achieving their dream of parenthood.
Support systems
Support systems play a crucial role in the journey toward conception for couples facing male infertility. They provide emotional, practical, and informational assistance, contributing to the well-being and resilience of individuals and couples.
- Partner support
Partners are often the primary source of support, offering emotional comfort, encouragement, and practical help during fertility treatments. Their understanding and empathy can significantly impact the couple’s ability to cope with the challenges of infertility.
- Family and friends
Family and close friends can provide a network of support, offering emotional encouragement, practical assistance with daily tasks, and a sense of belonging. Their presence can reduce stress and provide a buffer against the emotional toll of infertility.
- Healthcare professionals
Healthcare professionals, including doctors, nurses, and therapists, offer medical guidance, emotional support, and counseling. They provide information about treatment options, manage expectations, and help couples navigate the complexities of infertility.
- Support groups
Support groups connect individuals and couples with others going through similar experiences. They provide a platform for sharing knowledge, offering emotional support, and reducing feelings of isolation. Participation in support groups can foster a sense of community and empower couples.
These support systems are vital for couples facing male infertility. They offer emotional comfort, practical assistance, and a sense of community. By providing a supportive environment, they can enhance the well-being and resilience of individuals and couples, ultimately increasing their chances of achieving pregnancy and building a family.
Treatment options
Treatment options for male infertility encompass a range of medical and surgical interventions aimed at improving sperm production, function, or delivery. These options are tailored to the specific underlying cause of infertility, offering hope for couples seeking to conceive.
- Medication
Medications such as clomiphene citrate or gonadotropins can stimulate sperm production in men with hormonal imbalances or low sperm count.
- Surgery
Surgical procedures like varicocelectomy or vasectomy reversal can address physical blockages or abnormalities that hinder sperm transport.
- Assisted Reproductive Technologies (ART)
ART procedures, such as intrauterine insemination (IUI) or in vitro fertilization (IVF), bypass natural barriers and facilitate sperm-egg interaction.
- Lifestyle modifications
Adopting healthy lifestyle changes, including quitting smoking, reducing alcohol intake, and maintaining a balanced diet, can improve sperm quality and overall reproductive health.
The choice of treatment option depends on the underlying cause of infertility, the couple’s preferences, and the success rates associated with each approach. By exploring these treatment options, couples can increase their chances of achieving pregnancy and building a family.
Male Infertility FAQs
This FAQ section addresses commonly asked questions and provides clear answers to help individuals and couples better understand male infertility and available treatment options.
Question 1: What are the common causes of male infertility?
Answer: Male infertility can result from various factors, including hormonal imbalances, genetic abnormalities, lifestyle choices, and certain medical conditions that affect sperm production, motility, or delivery.
Question 2: How is male infertility diagnosed?
Answer: Diagnosis involves a physical examination, semen analysis, and medical history review. Additional tests, such as hormone level evaluation or genetic testing, may be recommended to determine the underlying cause.
Question 3: What are the treatment options for male infertility?
Answer: Treatment options vary depending on the cause of infertility and may include medication, surgery, assisted reproductive technologies (ART), or lifestyle modifications.
Question 4: Can male infertility be prevented?
Answer: While some causes of male infertility are preventable, such as avoiding excessive alcohol consumption and smoking, others may not be. Regular checkups and maintaining a healthy lifestyle can help reduce the risk of developing certain preventable causes.
Question 5: What is the success rate of male infertility treatment?
Answer: Success rates vary depending on the underlying cause, treatment approach, and individual factors. Some treatments may have higher success rates than others.
Question 6: What emotional challenges can couples face during infertility treatment?
Answer: Infertility can be emotionally challenging, causing stress, anxiety, and relationship strain. Seeking support from partners, family, friends, or support groups can provide emotional resilience.
These FAQs provide a general overview of male infertility and its management. Seeking personalized medical advice and support is essential for couples facing infertility and considering treatment options.
In the following section, we will delve deeper into the role of lifestyle factors and their impact on male fertility.
Tips for Improving Male Fertility
Lifestyle modifications can significantly impact male fertility. Here are five practical tips to enhance sperm health and increase the chances of conception:
Tip 1:Maintain a Healthy Weight
Obesity can negatively affect hormone levels and sperm production. Aim for a healthy weight range and consider consulting a healthcare professional for personalized advice.
Tip 2:Quit Smoking
Smoking damages sperm DNA and reduces sperm count. Quitting smoking improves sperm quality and overall reproductive health.
Tip 3:Limit Alcohol Intake
Excessive alcohol consumption can disrupt hormone production and sperm quality. Moderate alcohol intake or abstinence is recommended.
Tip 4:Follow a Balanced Diet
Include plenty of fruits, vegetables, and whole grains in your diet. Antioxidants and essential nutrients support sperm production and motility.
Tip 5:Exercise Regularly
Moderate exercise improves overall health and may enhance sperm count and motility. Avoid excessive or strenuous exercise, as it can have a negative impact.
Summary: By adopting these lifestyle modifications, men can improve their fertility potential. Maintaining a healthy weight, quitting smoking, limiting alcohol intake, eating a balanced diet, and exercising regularly contribute to optimal sperm production and quality.
These tips complement the medical and surgical treatment options discussed earlier, offering a holistic approach to managing male infertility and maximizing the chances of achieving pregnancy.
Conclusion
This comprehensive exploration of male infertility has shed light on the complexities of this condition and the multifaceted approaches to achieving pregnancy. Key takeaways include the importance of understanding the underlying causes of male infertility, ranging from genetic factors to lifestyle choices. The article emphasizes the significance of seeking medical advice and exploring treatment options, including medication, surgery, and assisted reproductive technologies, to address specific causes and improve fertility potential.
Moreover, the article highlights the crucial role of lifestyle modifications in enhancing male fertility. By maintaining a healthy weight, quitting smoking, limiting alcohol intake, adopting a balanced diet, and engaging in regular exercise, men can optimize sperm production and quality, thus increasing their chances of conception. These lifestyle adjustments complement medical interventions and provide a holistic approach to managing male infertility.