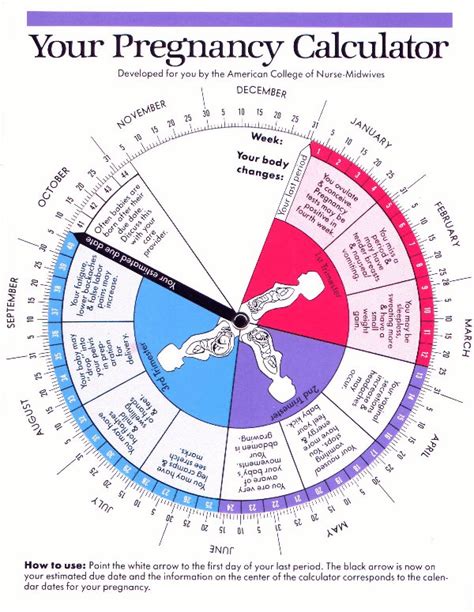
Calculating a pregnancy cycle is a critical step in monitoring the health and progress of both the expecting mother and developing child.
This calculation determines the estimated due date, guides prenatal care, and provides a timeline for the various stages of pregnancy. Historically, the Ngele rule, developed in the 19th century, provided a method to calculate the due date based on the mother’s last menstrual period.
In the following sections, we will explore the intricacies of calculating a pregnancy cycle, including methods for determining the expected delivery date, the factors that can influence its accuracy, and the significance of accurate pregnancy cycle calculation in ensuring optimal prenatal care.
How to Calculate Pregnancy Cycle
Calculating your pregnancy cycle accurately provides invaluable insights into the health of both the mother and the developing fetus. Here are ten key aspects that contribute to effective pregnancy cycle calculations:
- Last menstrual period (LMP)
- Ovulation date
- Conception date
- Gestational age
- Due date
- Ultrasound measurements
- Fetal heart rate
- Maternal symptoms
- Hormonal levels
- Medical history
By considering these aspects, healthcare professionals can determine the most accurate pregnancy cycle calculation for each individual patient. This information guides prenatal care, monitors the baby’s growth and development, and helps ensure a healthy pregnancy and delivery.
Last menstrual period (LMP)
In the context of calculating a pregnancy cycle, the last menstrual period (LMP) serves as a crucial reference point. Determining the LMP accurately is essential for estimating the gestational age and the expected due date.
- Timing: LMP refers to the first day of the woman’s last menstrual period.
- Cycle Length: The average menstrual cycle lasts for 28 days, but can vary from 21 to 35 days. Understanding the cycle length is important for calculating the ovulation date.
- Ovulation: Ovulation typically occurs 14 days before the start of the next menstrual period. This knowledge helps determine the approximate time of conception.
- Implantation: After ovulation, the fertilized egg takes about 6-12 days to implant in the uterus. Implantation marks the beginning of pregnancy.
By pinpointing the LMP and considering these factors, healthcare professionals can calculate a woman’s pregnancy cycle with greater accuracy. This information serves as the foundation for monitoring fetal development, scheduling prenatal appointments, and ensuring timely interventions if needed.
Ovulation date
In the context of calculating a pregnancy cycle, identifying the ovulation date is paramount. Ovulation marks the release of a mature egg from the ovary, creating the opportunity for fertilization and the subsequent journey of pregnancy.
- Timing: Ovulation typically occurs around day 14 of a 28-day menstrual cycle. However, it can vary depending on the individual’s cycle length.
- Hormonal surge: A surge in luteinizing hormone (LH) triggers ovulation. LH levels rise rapidly 24-36 hours before the egg is released.
- Physical signs: Some women experience physical signs of ovulation, such as mittelschmerz (ovulation pain), changes in cervical mucus, or a slight rise in basal body temperature.
- Ovulation predictor kits: These kits detect the LH surge in urine, providing an indication of impending ovulation.
Accurately determining the ovulation date plays a crucial role in calculating the pregnancy cycle. It helps establish the estimated time of conception, which is essential for monitoring fetal development, scheduling prenatal appointments, and ensuring timely interventions when necessary.
Conception date
The conception date, marking the moment when the sperm fertilizes the egg, represents a pivotal point in the journey of pregnancy. Accurately determining the conception date is crucial for calculating the pregnancy cycle, as it serves as the foundation for estimating the gestational age and the expected due date.
Establishing the conception date involves considering several factors. The most common approach is to count back from the estimated due date, presuming a typical gestational period of 40 weeks. Alternatively, if the woman remembers the date of ovulation, adding 14 days (the time it takes for the egg to travel through the fallopian tube and implant in the uterus) can provide an approximation of the conception date.
Knowing the conception date has several practical applications. It helps healthcare professionals monitor the progress of the pregnancy, assess fetal growth and development, and schedule prenatal appointments accordingly. Furthermore, in cases of high-risk pregnancies or potential complications, determining the conception date can aid in making informed decisions regarding medical interventions and specialized care.
Gestational age
Gestational age, a critical component of calculating a pregnancy cycle, refers to the duration of pregnancy from the first day of the woman’s last menstrual period (LMP) to the estimated date of delivery. Accurately determining gestational age is essential for monitoring fetal development, assessing pregnancy risks, and making informed decisions regarding prenatal care and delivery planning.
Gestational age is calculated using various methods, including ultrasound measurements, which provide precise estimates based on fetal size and development. Other factors considered include the woman’s menstrual history, ovulation date, and conception date. By combining this information, healthcare professionals can establish the most accurate gestational age for each individual pregnancy.
Understanding gestational age has several practical applications. It helps determine the appropriate timing for prenatal screenings, such as ultrasound examinations and blood tests, which assess fetal growth and well-being. Additionally, gestational age guides decisions regarding the management of high-risk pregnancies, including interventions such as bed rest, medication, or even preterm delivery in certain cases. Accurate gestational age calculation also facilitates the estimation of the expected due date, allowing for planning of delivery and postnatal care.
Due date
The due date, a critical component of calculating a pregnancy cycle, holds immense significance in prenatal care and delivery planning. It represents the estimated day when the baby is expected to be born and is calculated based on the woman’s last menstrual period (LMP) or the estimated date of conception.
Accurately calculating the due date is essential for several reasons. First, it helps healthcare providers monitor the progress of the pregnancy, assess fetal growth and development, and schedule prenatal appointments accordingly. Knowing the due date allows for timely interventions if any complications arise during the pregnancy.
Furthermore, the due date is crucial for planning the delivery. It helps determine the appropriate time for induction or cesarean section if necessary, ensuring the safety of both the mother and the baby. Additionally, knowing the due date allows families to make necessary arrangements for the baby’s arrival, such as preparing the nursery, purchasing essential items, and arranging for childcare or maternity leave.
Ultrasound measurements
Ultrasound measurements play a crucial role in calculating a pregnancy cycle and monitoring fetal development. Ultrasound technology emits high-frequency sound waves that bounce off the developing fetus, creating images that allow healthcare providers to visualize and measure various parameters.
These measurements, taken at different stages of pregnancy, provide valuable information about the fetus’s growth and well-being. By measuring the fetal head circumference, abdominal circumference, and femur length, healthcare providers can assess the fetus’s size and growth rate. Additionally, ultrasound measurements can detect abnormalities in fetal development, identify multiple pregnancies, and evaluate the placenta and amniotic fluid.
The accuracy of ultrasound measurements is dependent on several factors, including the skill of the sonographer and the quality of the ultrasound equipment. However, when performed by experienced professionals using high-quality equipment, ultrasound measurements are considered a reliable method for calculating the pregnancy cycle and monitoring fetal development.
Fetal heart rate
In the context of calculating a pregnancy cycle, monitoring the fetal heart rate provides valuable insights into the well-being and development of the growing fetus.
- Baseline heart rate
The baseline heart rate of a fetus typically ranges from 110 to 160 beats per minute. Variations from this range may indicate potential issues or complications, prompting further medical evaluation.
- Heart rate variability
The variability in the fetal heart rate is a measure of the changes in the time between heartbeats. Normal heart rate variability indicates a healthy fetal nervous system, while abnormal patterns may suggest distress or other underlying conditions.
- Accelerations
Accelerations are temporary increases in the fetal heart rate that are often associated with fetal movement or stimulation. Consistent accelerations are generally considered a sign of fetal well-being.
- Decelerations
Decelerations, on the other hand, are temporary decreases in the fetal heart rate. They can be caused by various factors, including uterine contractions or fetal distress, and require careful monitoring and evaluation.
By analyzing the fetal heart rate and its components, healthcare professionals can gain valuable information about the fetus’s condition, detect potential problems early on, and make informed decisions regarding the management of the pregnancy.
Maternal symptoms
In the comprehensive calculation of a pregnancy cycle, meticulous attention to maternal symptoms is paramount. These physical and emotional changes experienced by the expectant mother provide valuable insights into the well-being of both the mother and the developing fetus.
- Nausea and vomiting
Commonly known as morning sickness, nausea and vomiting are prevalent symptoms during the early stages of pregnancy. While typically not a cause for concern, persistent or severe symptoms may warrant medical evaluation.
- Breast tenderness
Breast tenderness and enlargement are early indicators of hormonal changes during pregnancy. These symptoms typically subside as the pregnancy progresses.
- Fatigue
Increased levels of progesterone and other hormones can lead to fatigue, especially during the first trimester. Adequate rest and a balanced diet are crucial to manage this symptom.
- Frequent urination
As the uterus expands, it puts pressure on the bladder, resulting in frequent urination. This symptom usually persists throughout the pregnancy.
By closely monitoring maternal symptoms and correlating them with other factors, healthcare professionals can effectively calculate the pregnancy cycle, anticipate potential complications, and provide timely interventions to ensure a healthy pregnancy and delivery.
Hormonal levels
In the intricate process of calculating a pregnancy cycle, understanding the role of hormonal levels is paramount. Hormones, chemical messengers produced by various glands in the body, play a crucial role in regulating the menstrual cycle and the development of pregnancy.
The primary hormones involved in pregnancy are human chorionic gonadotropin (hCG), progesterone, and estrogen. hCG is produced by the developing embryo shortly after implantation and is responsible for maintaining the corpus luteum, which produces progesterone. Progesterone, in turn, prepares the uterine lining for implantation and supports the pregnancy by suppressing uterine contractions.
Estrogen, primarily produced by the placenta, contributes to the development of the uterus and breasts during pregnancy. It also plays a role in preparing the body for labor and delivery. By monitoring hormonal levels, particularly hCG and progesterone, healthcare professionals can assess the viability of the pregnancy and detect potential complications.
Medical history
In the comprehensive calculation of a pregnancy cycle, a thorough review of the mother’s medical history plays a pivotal role in assessing potential risks and tailoring appropriate prenatal care.
- Chronic conditions
Pre-existing chronic conditions, such as diabetes, hypertension, or thyroid disorders, can impact the course of pregnancy and require specialized monitoring and management.
- Previous pregnancies
Information about previous pregnancies, including gestational age, birth weight, and any complications, provides valuable insights into potential risks and helps shape current prenatal care.
- Surgical history
A history of major surgeries, particularly those involving the reproductive organs, may affect the pregnancy’s progression and delivery plan.
- Genetic factors
Family history of genetic disorders or birth defects can inform genetic counseling and prenatal testing decisions.
By carefully considering the mother’s medical history, healthcare providers can identify potential risks early on, develop individualized care plans, and ensure the best possible outcomes for both the mother and the developing fetus.
Frequently Asked Questions about Pregnancy Cycle Calculation
This section addresses common questions and misconceptions surrounding the calculation of a pregnancy cycle.
Question 1: When should I start calculating my pregnancy cycle?
Answer: The most accurate method is to start counting from the first day of your last menstrual period (LMP).
Question 2: How can I estimate my due date?
Answer: You can use Naegele’s rule: Add 7 days to the first day of your LMP, then subtract 3 months.
Question 3: What factors can affect the accuracy of my pregnancy cycle calculation?
Answer: Irregular menstrual cycles, hormonal imbalances, and certain medical conditions can influence accuracy.
Question 4: Why is it important to know my pregnancy cycle?
Answer: It helps schedule prenatal appointments, monitor fetal development, and estimate the due date.
Question 5: What are the different methods used to calculate a pregnancy cycle?
Answer: The LMP method, ovulation prediction, and ultrasound measurements are common methods.
Question 6: Can I calculate my pregnancy cycle if I have irregular periods?
Answer: Yes, but it may be less accurate. Consult a healthcare professional for guidance.
These FAQs provide a concise overview of the key aspects of calculating a pregnancy cycle. For further insights and detailed information, refer to the comprehensive article that follows.
Next: Understanding the Importance of Accurate Pregnancy Cycle Calculation
Tips for Calculating Your Pregnancy Cycle Accurately
Accurately calculating your pregnancy cycle is crucial for prenatal care, monitoring fetal development, and preparing for delivery. Here are five essential tips to ensure precise calculation:
Tip 1: Determine Your Last Menstrual Period (LMP)
Pinpoint the first day of your last menstrual period, as it serves as the starting point for calculating your pregnancy cycle.
Tip 2: Track Your Ovulation
Monitor your body for signs of ovulation, such as mittelschmerz (ovulation pain), changes in cervical mucus, or a slight rise in basal body temperature.
Tip 3: Use an Ovulation Predictor Kit
These kits detect the surge in luteinizing hormone (LH) that precedes ovulation, providing an indication of your fertile window.
Tip 4: Consider Your Cycle Length
Understanding the average length of your menstrual cycles helps estimate the date of ovulation and conception.
Tip 5: Consult a Healthcare Professional
If you have irregular periods or difficulty determining your ovulation date, seek guidance from a healthcare provider for accurate pregnancy cycle calculation.
By following these tips, you can effectively calculate your pregnancy cycle, ensuring optimal prenatal care and peace of mind throughout your pregnancy journey.
Next: The Significance of Accurate Pregnancy Cycle Calculation
Conclusion
Throughout this comprehensive exploration of pregnancy cycle calculation, we have delved into various methods and factors that contribute to its accuracy. Key points to remember include:
- The significance of accurately determining the last menstrual period (LMP) as the cornerstone of pregnancy cycle calculation.
- The role of ovulation tracking and understanding menstrual cycle length in refining the estimation of conception.
- The importance of seeking professional guidance when faced with irregular periods or challenges in determining ovulation.
Calculating a pregnancy cycle with precision is not merely an academic exercise; it holds profound implications for prenatal care, fetal well-being, and delivery planning. By empowering individuals with the knowledge and tools to accurately determine their pregnancy cycle, we foster a proactive approach to reproductive health and promote positive outcomes for both mother and child.